Congenital Diaphragmatic Hernia
 The wide, flat muscle that separates the chest and abdominal cavities is called the diaphragm. The diaphragm forms over the course of the 6th through 12th weeks' gestation in the fetus. When it does not form completely, a defect, called congenital diaphragmatic hernia (CDH), is created. This defect or hole in the diaphragm muscle.
The wide, flat muscle that separates the chest and abdominal cavities is called the diaphragm. The diaphragm forms over the course of the 6th through 12th weeks' gestation in the fetus. When it does not form completely, a defect, called congenital diaphragmatic hernia (CDH), is created. This defect or hole in the diaphragm muscle.
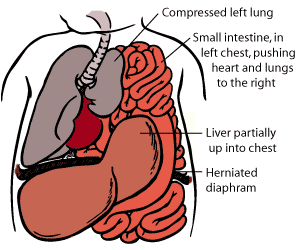
CDH occurs most commonly on the left side. The hole allows the contents of the abdomen (which may include the stomach, intestine, liver, spleen, or kidney) to go up into the fetal chest. The herniation of these abdominal organs into the chest occupies that space and prevents the lungs from growing to normal size. The growth of both lungs can be affected. This is called pulmonary hypoplasia.
While in the uterus, a fetus does not need its lungs to breathe, because the placenta performs this function. However, if the lungs are too small after the baby is born, the baby will not be able to provide itself with enough oxygen to survive.
Prenatal diagnosis & fetal treatment of CDH
CDH is typically diagnosed before birth during routine screening tests. Once this initial diagnosis is made it is important to get an expert assessment of your fetus's condition in order to determine the severity. The severity of your fetus's condition is an important guideline for determining the best treatment options.
Most fetuses with CDH require some level of prenatal monitoring. Care must be taken when choosing where to deliver the baby. Families will want to work out a plan for delivery and postnatal care with their obstetrician/perinatologist, the neonatologist, and pediatric surgeons so the baby can be stabilized and treated in the same center.
Fetuses on the most severe end of the spectrum with liver up into the chest and lung-to-heart ratio (LHR) less than 1.0 may be candidates for prenatal intervention, including fetoscopic balloon tracheal occlusion. More detailed information about prenatal testing, diagnosis, and fetal treatment for CDH can be found at Fetal Treatment Center: Congenital Diaphragmatic Hernia.
What is the outcome for a child with CDH?
There is a wide range of severity and outcomes for CDH. In the best cases, some infants do very well with routine neontal and surgical treatment after birth. Even though the lung isn't of normal size at birth, it has the capacity to grow and adapt for many years, so these children can lead normal active lives without restriction.
On the other end of the spectrum, babies with severe CDH and very small lungs are guaranteed to have a difficult struggle after birth, and some will not survive. Even when the CDH is severe, greater than 70% of affected babies can be saved with intensive support. However, there are often long term health issues related to breathing, feeding, growth, hearing, and development.
Most fetuses with CDH fall somewhere in-between these extremes of severity. For more information, read our page on CDH Long-Term Complications.
Delivery management of CDH
Babies on the better end of the spectrum have an excellent chance to lead a perfectly normal life. They do not require special prenatal management in terms of the timing or type of delivery, but should be delivered in a perinatal center with a Level III intensive care nursery with experienced neonatal and pediatric surgery providers. The place of delivery is very important because transporting these babies after birth can be dangerous for the infant. Most babies will be in the intensive care nursery for several weeks.
Babies diagnosised with severe CDH require very skilled intensive care to stay alive: high-frequency oscillatory ventilation, inhaled nitric oxide and, in some cases, extracorporeal membrane oxygenation (ECMO). ECMO provides temporary support for lung failure by circulating the baby's blood through a heart-lung type of machine. It can be life-saving, but can be used for only limited time before complications become excessive. These babies must be delivered in a very experienced tertiary perinatal center with ECMO capability.
After-birth surgical repair of CDH

 The surgery to repair diaphragmatic hernia after birth is not an emergency and is usually performed after the baby has stabilized in the first week of life. After repair, these babies will need intensive support for many weeks or even months.
The surgery to repair diaphragmatic hernia after birth is not an emergency and is usually performed after the baby has stabilized in the first week of life. After repair, these babies will need intensive support for many weeks or even months.
The severity and exact location of the hernia are evaluated by the surgeon at the time of the operation. Based on these findings, the hernia will be repaired in one of three ways. If the opening in the diaphragm is small and the amount of diaphragmatic muscle is adequate, the hole can be sewn closed. This is called a primary repair.
If the opening in the diaphragm is large or a significant portion of the diaphragm is absent, the surgeon will require additional tissue or material to close the defect. Often, a synthetic biocompatible material will be used to patch the opening-called a patch repair. In some patients, the surgeon will close the hole in the diaphragm with a flap of muscle-the internal oblique or latissimus dorsi from the infant's abdomen/back. This is called a muscle flap repair. In select circumstances, infants may be a candidate for a minimally invasive thoracoscopic repair. The surgeon will determine the type of repair required and the material to be used, at the time of the operation.
Follow up medical appointments & long-term care
A discharge summary of your child's hospital stay will be sent to your pediatrician. We recommend that you see your pediatrician within one week of leaving the hospital. We will make an appointment for your child to have their first visit in our long-term Multidisciplinary CDH Clinic soon after discharge. For questions before and in between appointments you may call the pediatric surgical office.
Long Term CDH Complications
How a baby with congenital diaphragmatic hernia recovers after birth is determined by many factors. Babies who experienced more severe CDH may face challenges which can include mild learning problems, breathing illnesses, hearing loss, and growth problems.
CDH recurrence
Some children require subsequent operation(s) to repair a recurrence of the CDH. Often this is related to the severity of the CDH at birth, and whether or not a synthetic patch was required to close the hole in the diaphragm. In our experience recurrence is less common for children with a primary repair and more common in children that require a patch repair. The patch may pull away from the chest wall, as the child grows, causing a recurrence.
The symptoms of a recurrence include retching, gagging and vomiting feedings, pain, or rapid breathing. Some children will have no symptoms. If you suspect a recurrence, take your child to the emergency room and explain your child's history and your suspicions to the emergency room team. You and the emergency room physicians can contact our surgeons at anytime.
Respiratory issues
Infants with CDH often have respiratory problems. This is due to impairment in lung growth (lung hypoplasia) which occurs before birth. Some children with respiratory problems may require supplemental oxygen at home. Supplemental oxygen helps to maintain a normal blood oxygen level and decreases the work of breathing (sparing calories needed for growth).
Some children fatigue easily with exercise or have respiratory problems such as asthma that improve with breathing medications.
Respiratory Syncytial Virus (RSV)
Children with CDH do not have normal lung development and are more susceptible to Respiratory Syncytial Virus (RSV) infections. RSV is a common cold virus that infects many people each winter. Children are thought to be most vulnerable in the first few years of life. For these reasons we recommend that your child receive Synagis® to prevent RSV infection during the first winter of life, at a minimum. This injection is given monthly during RSV season, usually November through March. If your child is in the ICN during the winter, the first dose can be given in the hospital before discharge and the remainder of the injection given outpatient.
Pulmonary Hypertension
Blood flow to the lungs of a fetus, is limited since breathing is not necessary. Once born, the blood flow to the lungs increases as the blood vessels gradually relax. If the blood vessels stay narrowed or "constricted", breathing can be difficult, even on a ventilator. This condition is called pulmonary hypertension. Newborns with CDH can have pulmonary hypertension that persists beyond for a few weeks to, rarely, many months after birth. This is monitored by echocardiogram in the ICN, and, if it doesn't resolve, evaluated by cardiac catheterization. These infants will be seen in the pulmonary hypertension clinic after discharge for ongoing evaluation and management.
GastroIntestinal issues
Nutrition & oral aversion
Prior to surgical repair, children with CDH often need to be fed through their veins, since their intestines are not working properly yet. They can still receive calories, protein, vitamins, and minerals this way. After surgical repair, they can begin to receive nutrition through their gastrointestinal tract. Some children with CDH tire easily since they are working hard to breathe, so it is difficult to take in everything they need by mouth.
When children cannot take enough feedings by mouth to stay nourished and hydrated and grow, feeds by nasogastric tube may be necessary. Feeding tubes are used to give breast milk or formula and medications. A child can usually still eat by mouth with a feeding tube in place. The feeding tube can be used to supplement their feedings by mouth. A nasogastric tube can be managed and replaced in the home.
In some cases a child with CDH is not able to feed by mouth at all. This can happen for a variety of reasons, such as they are too weak or tired from the surgery, or they are not able to safely take foods by mouth without coughing or choking. In these cases the child may need a more long term feeding tube called a gastrostomy tube. If the pediatric surgeon determines that your child will need a feeding tube for longer than a few weeks, a surgically placed gastrostomy tube may be required. Placement of a gastrostomy tube is a very routine procedure and usually does not require a lengthy hospital stay.
All children with CDH require more food, and more calories, than children without CDH. This is because children with CDH are working harder to breathe, and are working to develop their lungs after they are born, rather than in utero. Most often children with CDH need breast milk or formula that is more concentrated than normal. This can be prepared at home with a recipe you would receive from your dietitian. Even as children with CDH grow older, they still require higher calorie intake than their peers. In general they will follow a high calorie, high protein diet for most of their childhood.
Many children with CDH experience difficulty with feeding related to retching and reflux (see below). Sometimes dietary changes are used to manage these difficulties. For example, providing smaller, more frequent feedings or providing feedings at a slow, continuous rate. Feeding therapy by an occupational therapist can also help in severe cases.
Gastroesophageal reflux disease (GERD) & Fundoplication
Children with CDH frequently suffer from gastroesophageal reflux disease or GERD. Reflux means stomach contents reflux or back-up from the stomach into the esophagus. Gastroesophageal reflux can cause vomiting, heart burn and pain with feeding, breathing problems including pneumonia, apnea (periods of breath holding) and poor growth. Since GERD is so common in CDH patients, most CDH patients take antireflux medications for some time. In severe cases, a fundoplication may be recommended. Fundoplication is the name of the antireflux operation that helps stop the reflux of stomach contents into the esophagus. This operation is done by wrapping the upper stomach around the bottom of the esophagus. This helps tighten the valve at the bottom of the esophagus so food and fluids enter the stomach but are prevented from refluxing up into the esophagus.
Abdominal pain & appendicitis
Children with CDH have an atypical intestinal position because the intestine that was in the chest was moved manually into the abdomen. The appendix is normally found in the right lower abdomen, however children with CDH may have the appendix is a different location, depending upon the position of the intestine after the operation. This is important to know in the event your child develops abdominal pain and appendicitis is suspected. You should inform the providers caring for you child that he or she has a history of CDH and his or intestines are not rotated normally.
Constipation
For reasons that are not known, children with CDH frequently suffer from constipation. This is relieved with regular pediatric laxatives.
Bowel obstruction
Before the CDH operation, some of your child's abdominal organs were in the chest. During the operation the surgeon moved these organs into the abdomen and repaired the opening in the diaphragm. Because of this operation your child may form adhesions, or scar tissue within the abdomen that can kink the bowel. This kink will block the flow of liquid in the intestines. This is called a bowel obstruction. Signs of a bowel obstruction are green vomiting, pain and crying, abdominal distension and poor appetite. This is a serious problem and is considered an emergency. If your child develops these symptoms take your child to the emergency room. The emergency room physicians can contact our surgeons at anytime.
Problems with skeletal development
Scoliosis
Children with CDH can develop scoliosis or a curve in the spine as they grow. This may be related to differences in the two sides of the chest in children with CDH. Since the lung on the side of the CDH smaller, this may cause the spine to curve to that side. Also, the chest is smaller on the side of the CDH, which may contribute to the curvature of the spine. If your child develops scoliosis, he or she will be referred to an orthopedic surgeon for an evaluation.
Pectus chest wall deformity
Some children with CDH may develop a depression of the sternum, or breastbone. This is called a pectus excavatum. This may occur as a result of the increased work of breathing or differences in the two sides of the chest. This condition does not occur only in children with CDH. In most children, this causes no health risk however it will be monitored by the surgeon in the CDH clinic.
Hearing screening
Children who have been intubated on a ventilator with supplemental oxygen, received multiple medications, or have been treated with ECMO are at risk for hearing loss. Hearing tests are performed in the Intensive Care Nursery (ICN) before discharge. Because hearing loss may develop over many months, follow-up testing will be ordered after discharge by the CDH nursing coordinator. These hearing tests may be done at UCSF or at a hearing center near your home. Once the hearing test is performed and the results are available, the hearing center staff will recommend a schedule for follow up tests.
Developmental delay
Children who have been ill and hospitalized for prolonged periods are at risk for delay in normal development. It is important to identify any developmental delay as early as possible in order to begin treatment in a timely manner to maximize your child's potential. Our developmental pediatricians will assess and document your child's development at intervals during the first 5 years of life. The developmental pediatricians will make recommendations and referrals for services in your community.
CDH Homecare
We realize that having an infant with congenital diaphragmatic hernia (CDH) brings special challenges to your family. Your child may have long term complications due to CDH. The information below provides information to help you prepare for your child's care at home, and to answer questions you may have about your child's future.
LIFE Clinic - long-term follow-up care
Once your child is home, we wish to closely monitor your child's progress, in our outpatient multidisciplinary Congenital Diaphragmatic Hernia clinic, LIFE Program. Our specialists have specific expertise in the care of children with CDH and can provide continued care for your child. Team members include experts from Pediatric Surgery, Neonatology, Pulmonology, Nutrition, Developmental Pediatrics, Gastroenterology, Social Services and Nursing. An appointment will be made for your child in our CDH clinic prior to discharge.
Home nursing visits
You may be eligible for home nursing visits to help you learn how to care for your child at home. This referral will be made before you take you baby home from the hospital. Once you are home, the nurse will call you to make an appointment.
Home care supplies
Before your child's discharge home from the hospital, the ICN discharge planner will assist you in making the transition home. She will order any necessary supplies/equipment from a company your insurance carrier authorizes. These supplies include oxygen, feeding pumps, and gastrostomy supplies. These supplies will be sent to your home each month. The home care supply company will need to speak with you before sending the next month's shipment. Please contact the company at least one week from when you expect to need a new shipment so supplies do not run out.
Growth, Feeding, and Nutrition
One of the most important factors keeping your child well is adequate nutrition. Your child may require additional calories because increased work of breathing requires effort and uses energy. Additional calories can be given by offering more feedings, more concentrated feedings, or adding calorie supplements to feedings. Your child's growth will be monitored carefully in the intensive care nursery and after discharge. A pediatric nutritionist will create an individual feeding plan for your child based on his or her growth.
Formula and breast milk
If you are giving your child formula, the pediatric nutritionist will help you determine the best formula choice for your child. Most formulas contain 20 calories per ounce. Some children with CDH need feedings that are more concentrated than 20 calories per ounce. If your child needs concentrated formula, the pediatric nutritionist will provide you with instructions to mix your child's feedings to a specific concentration. It is important to follow the instructions carefully in order to mix feedings safely. If the formula and feeding plan is changed, and your child develops gagging, vomiting, gassiness or diarrhea please contact our office.
Vitamin supplements
Vitamin and iron supplements may be prescribed depending upon the type of feedings your baby is taking and whether or not he or she was born prematurely. The pediatric nutritionist and neonatologist will work together to determine what your child should receive at home. Please feel free to discuss this with your child's pediatric nutritionist or neonatologist.
Oral aversion and gastroesophageal reflux
Infants with CDH can develop symptoms of oral aversion, the refusal or inability to take feedings by mouth. If your child develops oral aversion it is important that you know this is not a failure on your part. There are many reasons this can happen. First, children who are ill and hospitalized for a prolonged period of time do not have the opportunity to practice feeding immediately after birth. This delays development of the skills needed to easily feed. Also, some children with CDH have severe gastroesophageal reflux. This may lead to esophageal irritation and pain with feeding.
Children with significant oral aversion will require a nasogastric tube or gastrostomy tube to deliver supplemental feedings until they are able to take all feedings by mouth. Children with oral aversion benefit from feeding therapy or occupational therapy. We have therapists available in our clinic to help you encourage your child to take feedings by mouth. Often occupational therapists are available in your community, close to home, through the local regional center in your area. We will make referrals for feeding therapy to help your child learn to take feedings by mouth. Fortunately most of our patients outgrow this problem but a small group of children may require feeding assistance for many years.
Feeding tubes: nasogastric and gastrostomy tubes
Feeding plans are individualized and vary from child to child. Some children with feeding tubes will need feedings delivered every few hours by a syringe, (called bolus feeding) and others will need feedings delivered over many hours by pump, called continuous feedings. Some children will receive feedings both by mouth and feeding tube, if oral feedings alone are inadequate.
If your child has a feeding tube, supplies and equipment will be ordered by the discharge planner in the ICN. It is important for you to know the name and phone number of the supply company as well as the list of supplies your child needs. Each month, it will be necessary to call the supply company to request shipment of the following month's supplies. Failure to do so may result in a delay in shipment of these important items.
Once you are home, the length of time your child will need the nasogastric or gastrostomy tube depends on whether he or she can learn to take all feedings by mouth and gain weight. Some children are able to transition off of the feeding tube in a few months and other children will need a feeding tube for a few years or longer. We will follow your child closely with our pediatric surgeon, neonatologist, nutritionist and feeding therapist to determine when your child is ready to have the feeding tube removed.
Respiratory care & supplemental oxygen
It is important to remember that you are the expert on your child's normal breathing pattern. Before you leave the hospital you will learn how your child's chest moves with each breath, and you be able to recognize changes in this pattern. At your first pediatric appointment, share with your child's doctor, how your child appears when breathing normally.
You will learn to recognize when your child has increased effort with breathing, a color change, retractions or irritability. All of these changes suggest that your child may be experiencing a breathing problem. These difficulties can be aggrevated by an RSV infection (a common cold virus) or other problem. For these reasons we recommend that your child receive Synagis® to prevent RSV infection for at least the first winter of life.
Supplemental oxygen
Some children with respiratory problems may require supplemental oxygen at home. Arrangements for home oxygen will be made by the ICN discharge planner. A home care supply company will deliver oxygen tanks and supplies to your home. Instructions will be provided regarding the proper use of the equipment and supplies needed for oxygen therapy. Monitoring, changes or cessation of home oxygen will be ordered by a pulmonary specialist during outpatient appointments.
California Children's Services (CCS)
CCS is a statewide insurance program that treats children with specific heath conditions including CDH. CCS will authorize and pay for specific medical services and equipment provided by CCS approval specialists including those at UCSF. Children born at UCSF or cared for in the hospital at UCSF with CDH will have a referral made to CCS by our CCS office staff. Your child's social worker can provide more information about this program if you have questions.
For more information check out the website for California Children's Services
Common mediations
Your child will be discharged from the hospital on medications. Before you go home, you will be taught the name of each medication, the reason for giving the medication (how it will help your child), and the correct way to give the medication. Typical examples include vitamins, iron, antacids, antireflux agents, diuretics and medications to help relax the blood vessels in the lungs. You will be given prescriptions to take to your local pharmacy the day your child is discharged home.
Once you are home, the dose of each medication may need to be adjusted for growth. Please speak to your child's pediatrician about this. Your pediatrician may be able to change medication doses for your child or refer you to the specialist at UCSF who prescribed the medication and is following your child. It is helpful for you to bring all of your child's medications to each appointment at UCSF in order to keep doses and prescriptions accurate.
Ranitidine (Zantac)
- Used to treat gastroesophageal reflux disease
- Changes the pH of the stomach secretions from acid to alkaline
- Prevents symptoms and damage to the gastrointestinal tract caused by stomach acid or infection
Metoclopromide (Reglan)
- Used to prevent or treat nausea and vomiting
- Used to treat gastroesophageal reflux disease
- May improve feeding problems and spitting up
- Increases stomach emptying of food and decreases symptoms of nausea, vomiting, heartburn, and fullness
- Give this medicine 15-30 minutes before meals and at bedtime
Sildenafil (Viagra)
- Used to treat increased blood pressure in the lungs
- Can relax lung vessels
Bosentian
- Used to treat increase blood pressure in the lungs
- Can relax lung vessels
Furosemide (Lasix)
- Used to get rid of extra fluid
- Used to treat high blood pressure
- Used to improve a weakened heart
- Gets rid of extra salt and water in the body through the kidneys
Budesonide (Pulmicort)
- Used to treat asthma
- Used to relieve allergy symptoms
- Prevents or reduces irritation, inflammation, and swelling
Support Groups & Other Resources
Taking care of a child recovering from CDH repair can be difficult and at times discouraging. During your child's convalescence it is important for family members to relieve each other and for couples to
find time to be together. This may mean leaving your child in the care of another trusted adult, even if it's only for a few hours.
The comfort and support of other parents in similar circumstances cannot be underestimated. Referrals to resources in your local community will be made by the ICN team and CDH clinic personnel. Our team of specialists is here to help you through this challenging transition after your
child leaves the nursery.
More support resources can be found at the following non-profit groups:
- Cherubs - The Association of Congenital Diaphragmatic Hernia Research, Advocacy, and Support.
- Nayeli Faith Foundation - Offers financial assistance and support to CDH families at UCSF.
